


 |
 |
 |
 |
My PhD directors are Yohan Payan and Jocelyne Troccaz.
We work with:
- The biomechanics laboratory of Toulouse, with Pascal Swider, Annaig
Pedrono, Dominique Ambard and Fabien Audry.
- The maxillo facial surgery departement of the Toulouse hospital, with Franck
Boutault and Christophe Marecaux.
The exophthalmia is an orbitary pathology caracterised by an excessive forward
displacement of the eye ball. This displacement (called protrusion) is a
consequence of an increase of the orbital content behind the eye ball. The
exophthalmia consequences are aesthetical as well as psychological. Moreover,
some functional problems can appear, it is the case if exophthalmia leads to a
too long cornea exposition or if the optic nerve is distended (which implies a
decrease of the visual acuity) or broken. Four origins are known for
exophthalmia. First, following a trauma, an haematoma can compressed the optic
nerve which can reduce the visual perception. A surgical decompression of the
haematoma may then be necessary. The second exophthalmia cause is cancerous,
with tumour in one or both orbits that may reduce the mobility of the globe.
Radiotherapy can be used and surgical extraction of the tumour is sometimes
needed. Third cause of exophthalmia: infections, that are treated with
antibiotics. Finally, and for most cases, exophthalmia can be due to endocrinal
dysfunction, such as the Basedow illness which is related to a thyroid
pathology. This cause often leads to a bilateral exophthalmia as this
dysfunction induces an increase of the ocular muscles and fat tissues volume.
Once the endocrinal situation is stabilized, a surgical reduction of the
exophthalmia is usually needed. In our case, this reduction is made by a
decompression of the orbit. That is to say that the surgeon break the bony
structures (in the ethmoid or the maxillary sinuses regions) to increase the
volume of the orbital cavity. This gesture must be very precise and that is why
we propose to assist it with computer guided simulations.
The first step of my PhD has consisted in the creation of a visualisation tool
for CT scan exams or MRI exams. This tool, developed in Visual C++ and VTK,
allows to visualize the patient exams and to segment (with manual spline
segmentation) the orbit, the muscles and the optic nerve. Moreover, this tool
provides a 3D reconstruction of the studied structure and locate 2D scanner
points on the 3D models (and reciprocally). The goal is to facilitate the
surgical planning.
The second step of my work implies the biomechanics laboratory of Toulouse,
since it focuses on the biomechanics model of the orbital structures. Indeed,
from a pre operative exams (MRI or CT scan), the geometry of the intra orbital
components (eye ball, muscles, nerve, fat tissues) have been reconstructed and
have allowed to defined a base for the development of a 3D biomechanics model.
The final objective is to build a software with this model that could be used by
a surgeon (we work with the professor Franck Boutault, maxillo facial surgery
department of Purpan hospital) to predict the global behaviour of the eye ball
following the surgery (which induces bone geometry modifications) and especially
to predict the backward displacement of the eye ball during the decompression.
The third step consists in the development of a software able to locate surgical
tools during orbital surgery. The idea is to indicate to the surgeon the
localisation of the tool tips in different types of exams (MRI or CT scan)
corresponding to the patient. The surgeon has thus the possibility to plan his
intervention in the image exam (determination of the bony structures to break,
the nerve zone…) and to retrieve this planification during the surgery with the
localisation system. This step will be developed with the help of the PRAXIM
society.
To know more about the subject in MS Word format.
To see the work done during my PhD : click here.
This work has been done during my DEA IVR.
The general idea was to use matching process to get automatic volumic meshes of bonny structures.
For example, we worked with Beatrice Couteau, who realised during her PhD a Finite Element biomechanical model of a femur, based on
patient data. By using the matching process on this patient mesh with an other patient shape, we have automatically generated a mesh
associated to this new patient and thus a biomechanical model has been associated to it.
The aims of this work were:
(1) to evaluate the possibility to have an automatic procedure
(2) to see until which level of anatomical complexity this procedure cannot be automatic
(3) to propose solutions to improve our matching process to keep its automatic interest.
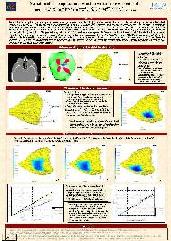
The evaluation of the matching process on few femurs has demonstrated that our program produced irregular meshes, that is to say they did
not satisfy the constraints required for a Finite Element analyse. A procedure of mesh correction has thus been programmed to regularized
those meshes. This process is based on criteria such as the Jacobian determinant or the warping factor. The regularisation step follows
an iterative way applying a correction to each irregular elements by moving each node according to the gradient of the Jacobian
determinant.
Publications and Proceedings

|
Version powerpoint |

|
Version powerpoint |
|
Version powerpoint |